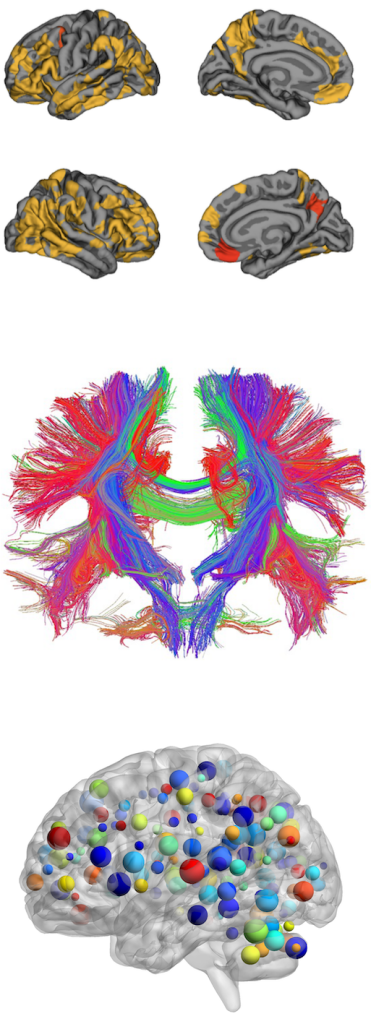
Neural Correlates of Speech, Hearing and Language Related Disorders
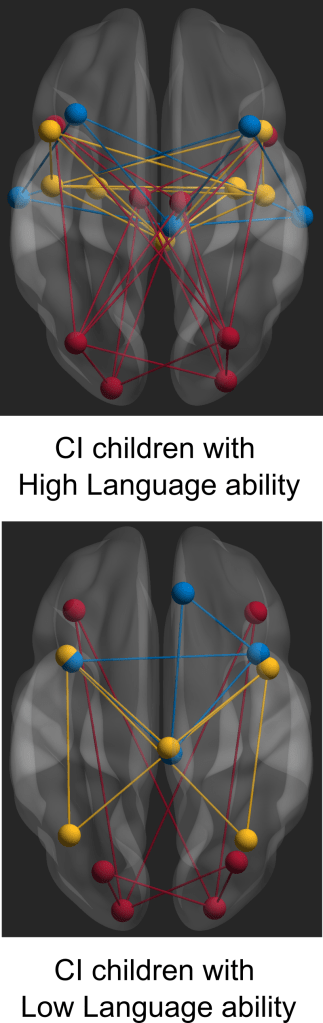
Neurodevelopmental processes such as neurogenesis, cell migration, and neuronal connectivity are implicated in a range of neurodevelopmental disorders. Hence in some of the recent work, I have been exploring ways to quantify these structural alterations in disorders mostly related to speech and language like stuttering and dyslexia along with the impact of hearing loss in the development of speech and language related functions. In a recent study related to reading ability, we were able to show that the white matter tissue architecture in the brain can inform etiological models of dyslexia and explain sources of individual differences in reading ability in children aged 5 to 17 years (Koirala et al. 2021). Similarly, for individuals who stutter, we provided evidence of a wide-spread reduction in white matter structural connectivity in the brain areas which are associated with anxiety, reinforcing the influence of a socio-emotional component (Koirala et al. 2022). In another recently published study that was highly relevant for neurodevelopmental research, we tested the quality of neuroimaging data collected from large sample of children with developmental disorders and its impact on the outcome measures (Koirala et al. 2022). Cochlear implantation (CI) in prelingually deafened children has been shown to be an effective intervention for developing language and reading skill. However, there is a substantial proportion of the children receiving CI who struggle with language and reading. In a recent studies, we identify the neural underpinnings in two groups of CI children with good and poor language and reading skills (Koirala et al. 2023, Deroche et al. 2023, Deroche et al. under review). These neural differences in the two groups of CI children may reflect potential biomarkers for predicting outcome success in CI children.
Please refer to the publication page for full text access of the citations.
Brain Imaging Biomarker for Neurodegenerative Disorders
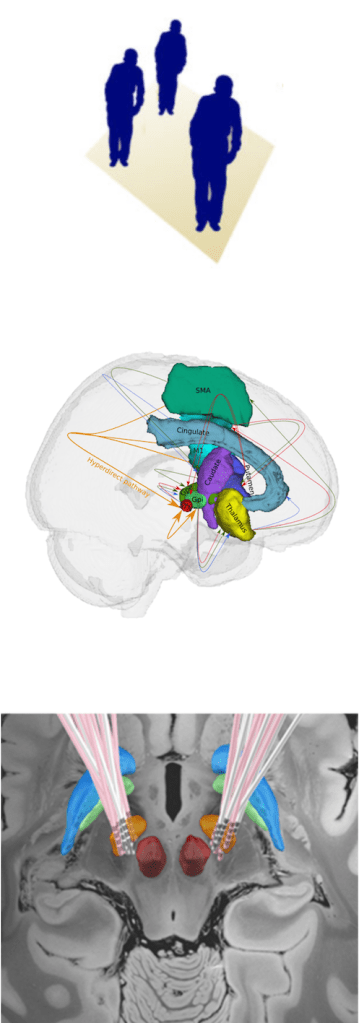
Movement disorders refers to group of neurological conditions with either an excess of movement or a paucity of voluntary and involuntary movements with age as one of main risk factor (Jankovic, Hallet & Fahn et al. 2011). As the global population is rapidly aging with an estimated 22% will be over 65 by 2050, it is becoming an unprecedented social and economic challenge. The estimated cost of global care for individuals with movement disorders is in trillions (e.g., 2017 cost estimate for individuals with PD only in US is $52 billions and projected to surpass $79 billions by 2037), and the number is ever growing with the aging population (Yang et al. 2020). Parkinson’s disease (PD) and Dystonia are one of the most common movement disorders with no permanent cure. Deep Brain Stimulation (DBS) is currently a standard evidence-based treatment for these patients that substantially improves the motor and non-motor symptoms. The actual cause of neurodegeneration as well as the precise mechanism of DBS is still not fully understood. Hence from the beginning days of my research, one of my primary interest was in understanding the pathophysiology of the disease and possibly the mechanism of the DBS and facilitate the diagnostics by developing clinically applicable non-invasive biomarkers. Over the years, we have been able to quantify the widespread brain network effects of Deep brain stimulation in Parkinson’s disease (Koirala et al. 2016, Koirala et al. 2020, Muthuraman et al. 2020) and Dystonia (Gonzalez-Escamilla et al. 2019, Chirumamilla et al. 2019), predict the outcome of the surgery or effect of treatment based on brain structural alterations and connectivity patterns (Hanganu et al. 2016, Muthuraman et al. 2017, Koirala et al. 2018, Muthuraman & Koirala et al. 2018) and classify the PD brain from healthy brain using white matter microstructural integrity (Koirala et al. 2019). Moreover, in other findings, we were able to evidence the brain network fingerprints of different types of tremors experienced by these patients (Muthuraman et al. 2018) which was selected as the Editor’s choice article in the Journal Brain and a simple spiral drawing technique that to be used for clinical diagnosis (Koirala et al. 2015).
Please refer to the publication page for full text access of the citations.
Brain Structure alterations and it’s impact on Pathophysiology
Brain structure changes as a result of various Psychological and Neurological disorders and also true the other way around – these disorders result in structural changes in the brain. The behavioral changes that we observe could be quantified in these disorders, but it always has this trailing question, So what exactly cause this changes? I believe that all the functional and behavioral adaptations are rooted to the micro or macro level structural alterations in the brain. These alterations could be anywhere in Grey matter, White matter or cerebrospinal fluid (CSF) and might indicate changes in neurite features, glial cells, fiber tracts, etc. Fortunately, with the non-invasive brain imaging techniques like T1-weighted, T2-weighted and Diffusion Weighted Imaging (DWI) which could be obtained using Magnetic Resonance Imaging (MRI) and electrophysiological measure like electroencephalography (EEG), electromyography (EMG) some of these changes could be investigated. Moreover, with the help of invasive and non-invasive stimulation techniques like Transcranial Magnetic Stimulation (TMS) and Deep Brain Stimulation (DBS) these effects could be modified. Hence, over the years, I was involved in the investigation of how some of these psychological and neurological disorder alters our brain structure and how it impacts the overall network level functioning of the brain. Over the years, we have evidenced these effects and the possibility of its modifications in neurological disorders like Multiple Sclerosis (Fleischer et al. 2016, Kroth et al. 2017, Fleischer & Koirala et al. 2019, Ciolac et al. 2019, Radetz et al. 2019, Cerina et al. 2020, Muthuraman et al. 2020), Migraine (Michels et al. 2019, Michels & Koirala et al. 2021), Epilepsy (Chiosa et al. 2017 & 2019) to neuropsychological events like fear processing (Chirumamilla et al. 2019, Gonzalez-Escamilla, Chirumamilla & Koirala et al. 2022).
Please refer to the publication page for full text access of the citations.